Today is officially the last day of Anna’s treatment for leukaemia.
Today is officially the last day of Anna’s treatment for leukaemia.
It is two years and two months since her diagnosis. She has had oral chemotherapy for most of those 789 days, regular intravenous and brain/spinal fluid chemotherapy, lumbar punctures, daily/weekly/monthly steroids and numerous blood transfusions.
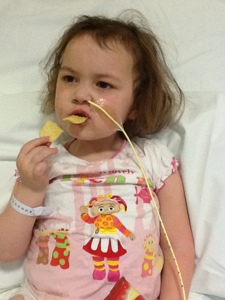
She’s had a portocath put under her skin, a feeding tube down her nose and one very unpleasant bronchial wash.
She has been on antibiotics, antivirals, antifungals, antiemetics and a cocktail of other drugs to counteract the side effects of all of the above. She has had IV fluids, electrolytes, overnight liquid feeds and saline drips.
Pain relief has ranged from calpol to morphine.
She is a frequent visitor to x-ray, and also had ultrasounds, ECGs, CT scans, MRIs and a bone density scan.
She is known to many of the departments at sick kids – neurology, endinocrology, respiratory, orthopaedic and oncology.
I’ve lost count of how many nights we’ve spent in hospital or how many outpatient appointments she’s had.
She still had some walking ability when she was diagnosed but now she isn’t able to bear any kind of weight at all. Her bones are like tissue paper and break with the slightest trauma. She has had seven fractures (femur, knees, ankles, feet, wrists). We have no idea if she will recover any strength.
She’s also had three bouts of shingles, staff epidermidis (at least twice), kiebseilla, para flu, cellulitis, mouth ulcers, UTIs, aspergillus, rsv, septic/deranged liver, various other bacterial/viral infections and an extremely severe skin reaction. And there have been a couple of times when we thought she might not make it.
Although today is a day of celebration, it’s also something of an anti-climax as her steroids were stopped some months ago due to her getting continued infections. She had her last dose of chemotherapy over a week ago as it was stopped due to her low platelets and currently we are in sick kids as she has several infections. She had a platelet transfusion this morning and needs a red blood cell transfusion tomorrow. She’s also had her monthly 4 hour pomidronate infusion today today – her bone strengthening treatment.
She was due to have her final bone marrow/lumbar puncture done today but wasn’t well enough. It will probably take place next week. She still needs to have one catch up intrathecal/general anaesthetic, likely to take place on fifth of March. We will continue to come to clinic regularly and she will be having pomidronate monthly.
However, we are glad to get to today. She is still my beautiful, gorgeous daughter and now we can start planning for the future – Anna, me and Nathan. X